Impact Factor ISSN: 1449-2288
Int J Biol Sci 2020; 16(6):947-956. doi:10.7150/ijbs.37861 This issue Cite
Research Paper
Vitamin A deficiency causes islet dysfunction by inducing islet stellate cell activation via cellular retinol binding protein 1
1. Department of Endocrinology, Zhongda Hospital, Institute of Diabetes, School of Medicine, Southeast University, Nanjing, China
2. Department of Gastroenterology, Jinling Hospital, Medical School of Nanjing University, Nanjing, China
3. State Key Laboratory of Bioelectronics, School of Biological Science and Medical Engineering, Southeast University, Nanjing, China
4. Department of Diabetes, School of Life Course Sciences, King's College London, Guy's Campus, London, UK
5. Department of Biochemistry and Molecular Biology, School of Medicine, Southeast University, Nanjing, China
Abstract
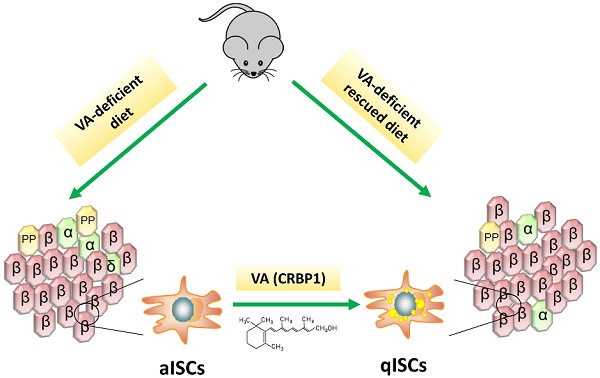
Background: Vitamin A (VA) plays an essential role in pancreatic homeostasis. Islet stellate cells (ISCs) are VA-storing cells in pancreatic islets. Herein, we have investigated the effect of VA on glucose homeostasis trough regulation of ISCs function in dietary VA deficiency model mice.
Methods: Male C57BL/6 mice were randomly fed a VA-sufficient, a VA-deficient (VAD) or a VAD-rescued diet. Glucose metabolism was assessed by glucose tolerance tests and immunohistochemistry. ISCs activation degree was evaluated by immunofluorescence, quantitative PCR and western blotting in both, retinol-treated cultured ISCs and model mice. Changes in ISCs phenotype and their effect on islets were assessed by lentiviral transduction and enzyme-linked immunosorbent assays in a co-culture system.
Results: VAD mice showed irregular shaped islet, glucose intolerance, islet size distribution excursions, and upregulated expression of α-smooth muscle actin (α-SMA, marker of ISCs activation). Reintroduction of dietary VA restored pancreatic VA levels, endocrine hormone profiles, and inhibited ISCs activation. Incubation with retinol increased the expression of VA signaling factors in ISCs, including cellular retinol binding protein 1 (CRBP1). The knockdown of CRBP1 maintained the quiescent ISCs phenotype and reduced the damage of activated ISCs on islet function.
Conclusions: VA deficiency reduced islet function by activating ISCs in VAD mice. Restoring ISCs quiescence via CRBP1 inhibition could reverse the impairment of islet function caused by activated ISCs exposure.
Keywords: vitamin A, β cell, islet stellate cell, activation, CRBP1

 Global reach, higher impact
Global reach, higher impact