Impact Factor ISSN: 1449-2288
Int J Biol Sci 2015; 11(2):156-167. doi:10.7150/ijbs.10283 This issue Cite
Research Paper
Effects of Nitric Oxide on Notexin-Induced Muscle Inflammatory Responses
1. Department of Anatomy, Guangdong Provincial Key Laboratory of Construction and Detection in Tissue Engineering, Southern Medical University, Guangzhou, 510515 China
2. Department of Emergency, NanFang Hospital, Southern Medical University, Guangzhou, 510515 China
* The first three authors contributed equally to this work
Abstract
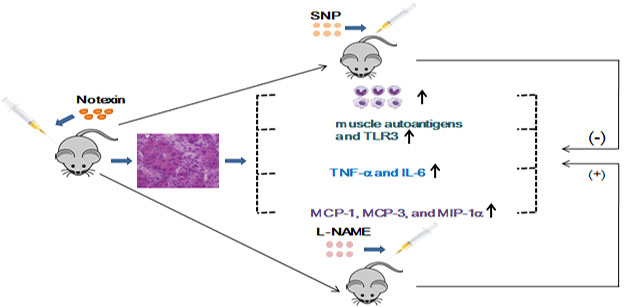
Excessive inflammatory response may delay the regeneration and damage the normal muscle fibers upon myoinjury. It would be important to be able to attenuate the inflammatory response and decrease inflammatory cells infiltration in order to improve muscle regeneration formation, resulting in better muscle functional recovery after myoinjury. This study was undertaken to explore the role of Nitric oxide (NO) during skeletal muscle inflammatory process, using a mouse model of Notexin induced myoinjury. Intramuscular injection (tibialis anterior, TA) of Notexin was performed for preparing mice myoinjury. NO synthase inhibitor (L-NAME) or NO donor (SNP) was intraperitoneally injected into model mice. On day 4 and 7 post-injury, expression of muscle-autoantigens and toll-like receptors (TLRs) was evaluated from muscle tissue by qRT-PCR and Western Blot; the intramuscular infiltration of monocytes/macrophage (CD11b+ or F4/80+ cells), CD8+ T cell (CD3ε+CD8α+), apoptotic cell (CD11b+caspase3+), and MHC-I molecule H-2Kb-expressing myofibers in damaged muscle were assessed by imunoflourecence analysis; the mRNAs expression of cytokines and chemokines associated with the preferential biological role during the muscle damage-induced inflammation response, were assessed by qRT-PCR. We detected the reduced monocytes/macrophages infiltration, and increased apoptotic cells in the damaged muscle treated with SNP comparing to untreatment. As well, SNP treatment down-regulated mRNA and protein levels of muscle autoantigens, TLR3, and mRNA levels of TNF-α, IL-6, MCP-1, MCP-3, and MIP-1α in damaged muscle. On the contrary, L-NAME induced more severe intramuscular infiltration of inflammatory cells, and mRNA level elevation of the above inflammatory mediators. Notably, we observed an increased number of MHC-I (H2-Kb) positive new myofibers, and of the infiltrated CD8+ T cells in damaged muscle at the day 7 after L-NAME treatment. The result herein shows that, NO can act as an endogenous anti-inflammatory molecule during the ongoing muscle inflammation. Our finding may provide new insight to optimize NO-based therapies for improving muscle regeneration after myoinjury.
Keywords: Nitric Oxide, inflammation, skeletal muscle

 Global reach, higher impact
Global reach, higher impact