Impact Factor ISSN: 1449-2288
Int J Biol Sci 2021; 17(3):683-688. doi:10.7150/ijbs.56037 This issue Cite
Research Paper
Depression and its relationship with quality of life in frontline psychiatric clinicians during the COVID-19 pandemic in China: a national survey
1. Department of Psychiatry, Xiamen Xianyue Hospital, Xiamen, China.
2. Unit of Psychiatry, Institute of Translational Medicine, Faculty of Health Sciences, University of Macau, Macao SAR, China.
3. Centre for Cognitive and Brain Sciences, & Institute of Advanced Studies in Humanities and Social Sciences, University of Macau, Macao SAR, China.
4. The National Clinical Research Center for Mental Disorders & Beijing Key Laboratory of Mental Disorders Beijing Anding Hospital & the Advanced Innovation Center for Human Brain Protection, Capital Medical University, School of Mental Health, Beijing, China.
5. Department of General Surgery, Beijing Liangxiang Hospital, Capital Medical University, Beijing, China.
6. School of Nursing, Hong Kong Polytechnic University, Hong Kong SAR, China.
7. Global and Community Mental Health Research Group, New York University (Shanghai), Shanghai PR China.
8. School of Global Public Health, New York University, NY, USA.
#These authors contributed equally to the work.
Abstract
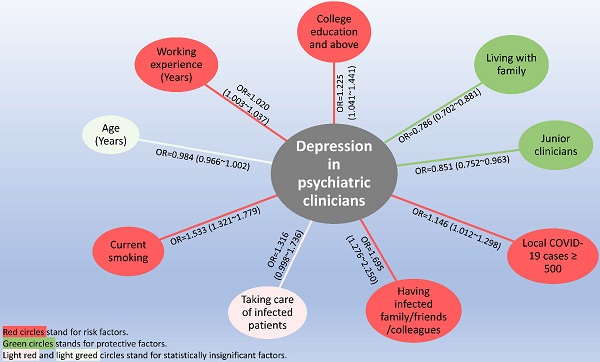
This was a national survey that determined the prevalence of depressive symptoms (depression thereafter) and its relationship with quality of life (QOL) in frontline clinicians working in psychiatric hospitals in China during the COVID-19 pandemic. Depression and QOL were assessed using the Patient Health Questionnaire nine items (PHQ-9) and the World Health Organization Quality of Life Questionnaire-brief version (WHOQOL-BREF), respectively. Multivariable logistic regression analyses and analysis of covariance were used. A total of 10,516 frontline clinicians participated in this study, of which, 28.52% (n=2,999) met screening criteria for depression. Compared to those without depression, clinicians with depression had a lower quality of life (F (1, 10515) =2874.66, P<0.001). Higher educational level (OR=1.225, P=0.014), if the number of COVID-19 patients in the hospital catchment area surpassed 500 (OR=1.146, P=0.032), having family/friends/colleagues who were infected (OR=1.695, P<0.001), being a current smoker (OR=1.533, P<0.001), and longer working hours (OR=1.020, P=0.022) were independently associated with higher risk of depression. Living with family members (OR=0.786, P<0.001), and being junior clinicians (OR=0.851, P=0.011) were independently associated with lower odds of depression. The results showed that depression was common in frontline psychiatric clinicians during the COVID-19 pandemic. Timely assessment and effective interventions of depression for frontline clinicians in psychiatric hospitals were warranted.
Keywords: COVID-19, depression, psychiatric clinician, quality of life, prevalence

 Global reach, higher impact
Global reach, higher impact